ACNE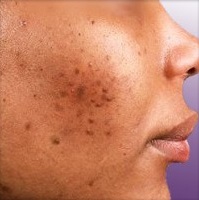 ON BLACK SKIN
ON BLACK SKIN
Acne is an extremely common dermatological condition since it affects about 80% of adolescents. In 20% of cases, it comes in its moderate to severe form. Known to occur at the approach of puberty, acne usually progresses to spontaneous healing around the age of 20 to 25. It should be noted, however, that for black and matte skin, the onset is gladly delayed at the age of 16 or 17 years, and the duration extended until the age of 25 to 30 years. Acne is therefore not only a dermatosis of the adolescent. Its prevalence in adults, estimated at 40%, is also increasing.
What is acne?
Acne is defined as a chronic disease related to inflammation of the pilosebaceous follicle. Its development takes place in three stages:
- Under hormonal dependence, stimulation of the sebaceous gland induces an overproduction of sebum (hyperseborrhea)
- Due to the abnormal proliferation of keratin, the excretory duct of the pilosebaceous follicle is blocked; sebum secreted upstream can no longer be evacuated to the surface of the skin, resulting in the formation of retentional lesions (open comedones or blackheads, closed comedones or microcysts)
- The bacterium Propionibacterium acnes proliferates in retentional lesions; its microbial activity plays a decisive role in the formation of inflammatory lesions (red papules or pimples, white pustules or pimples, nodules or red pimples, voluminous and painful)
Lesions and pimples are localized in the areas richest in sebaceous glands, that is, in the face, back, neck or chest.
When cured, acne leaves more or less deep and lasting marks. While it is true that some lesions disappear completely, others are the cause of indelible scars. When it comes to black and matte skin, scarring following acne is a problem in its own right. Indeed, on these particularly sensitive and reactive skin types, the slightest trauma such as a small pimple generates a transient stimulation of melanin production. This results in the appearance of
hyperpigmentation spots.
Although there is a genetic predisposition to acne, multiple factors can increase its risk or persistence. Thus, friction due to clothing, exposure to the sun, the use of fatty or occlusive cosmetics, stress, taking certain hormonal drugs, etc. are all elements aggravating acne breakouts and lesions. There are many cases where acne is caused by a slight hormonal imbalance, which is why it may be useful, in case of persistent acne, to make a hormonal assessment with your gynecologist.
How to treat acne?
The
treatment of acne depends on its severity. The comedon stage is less problematic to manage but can easily progress to an inflammatory form with a risk of scarring. The most severe form requires drug management by topical application (cream, gel, lotion) or systemically (capsule, tablet). This drug treatment combines retinoids, to fight against comedones by unclogging pores, with various compounds acting on inflammatory lesions (azelaic acid, topical corticosteroid, benzoyl peroxide, zinc gluconate and isotretinoin in the case of severe acne), as well as an antibiotic to prevent bacterial proliferation.
Treat acne with a three-care system:
 ON BLACK SKIN
ON BLACK SKIN

